Turn obesity population data into structured pathway action.
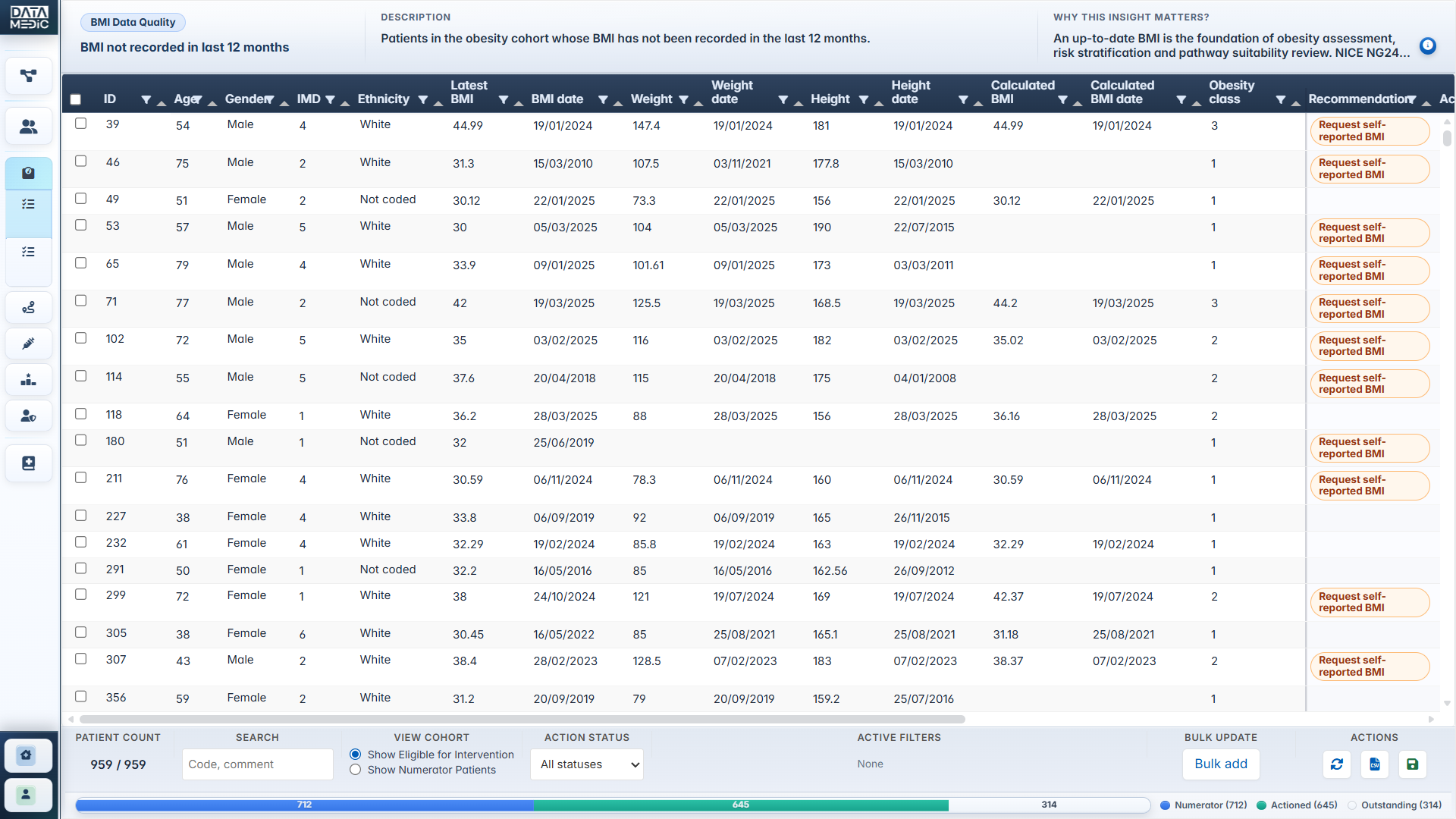
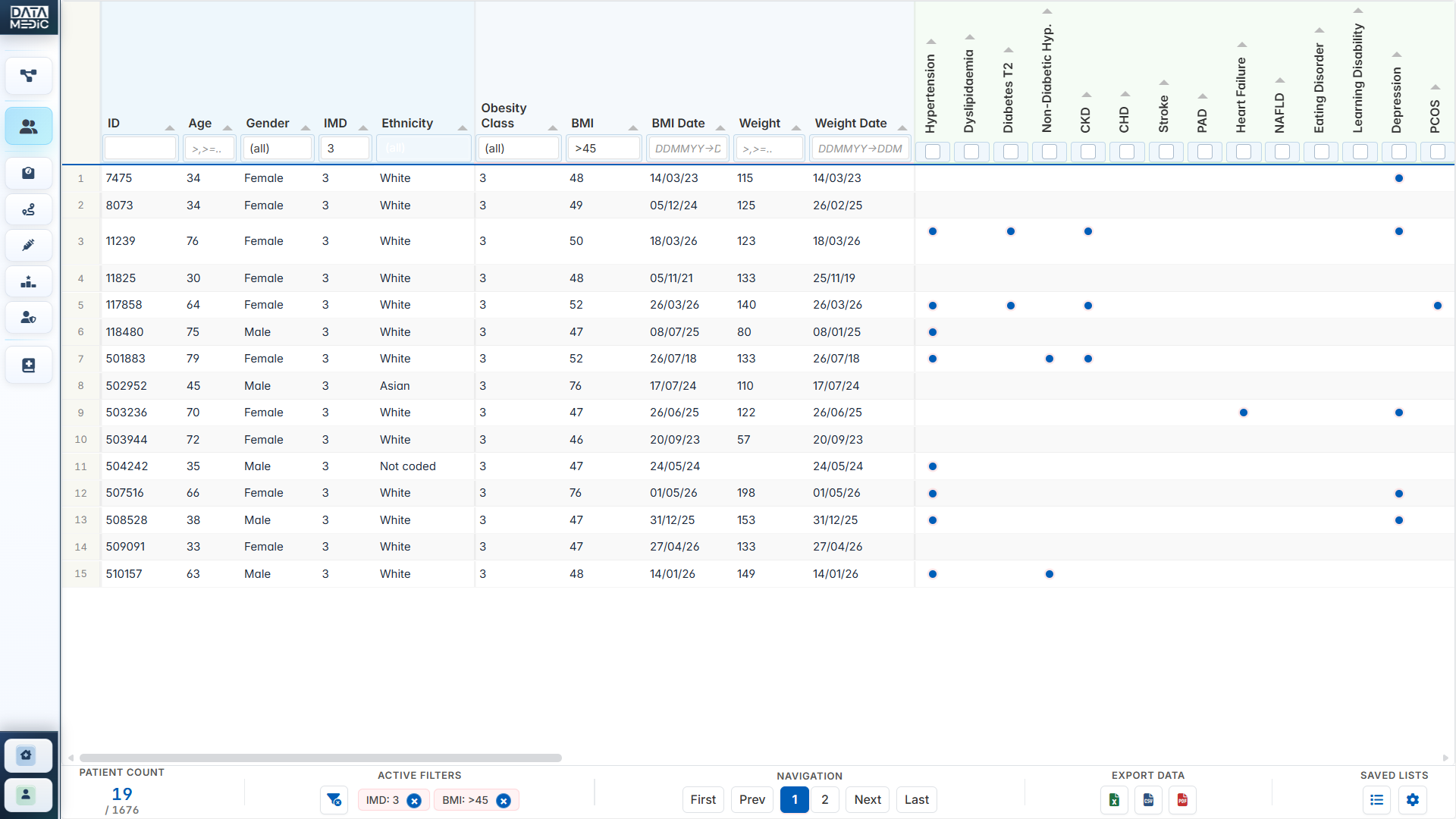
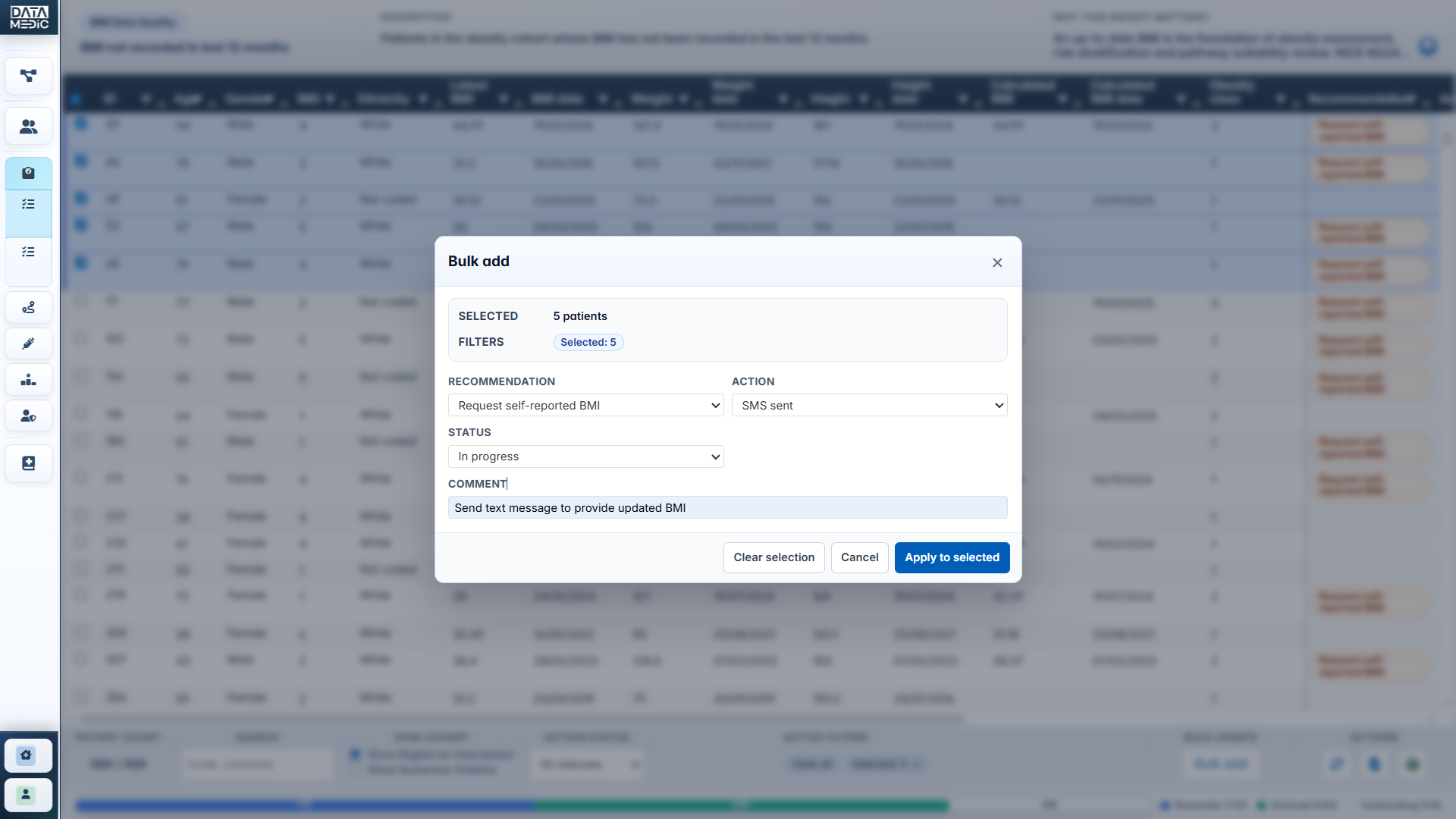
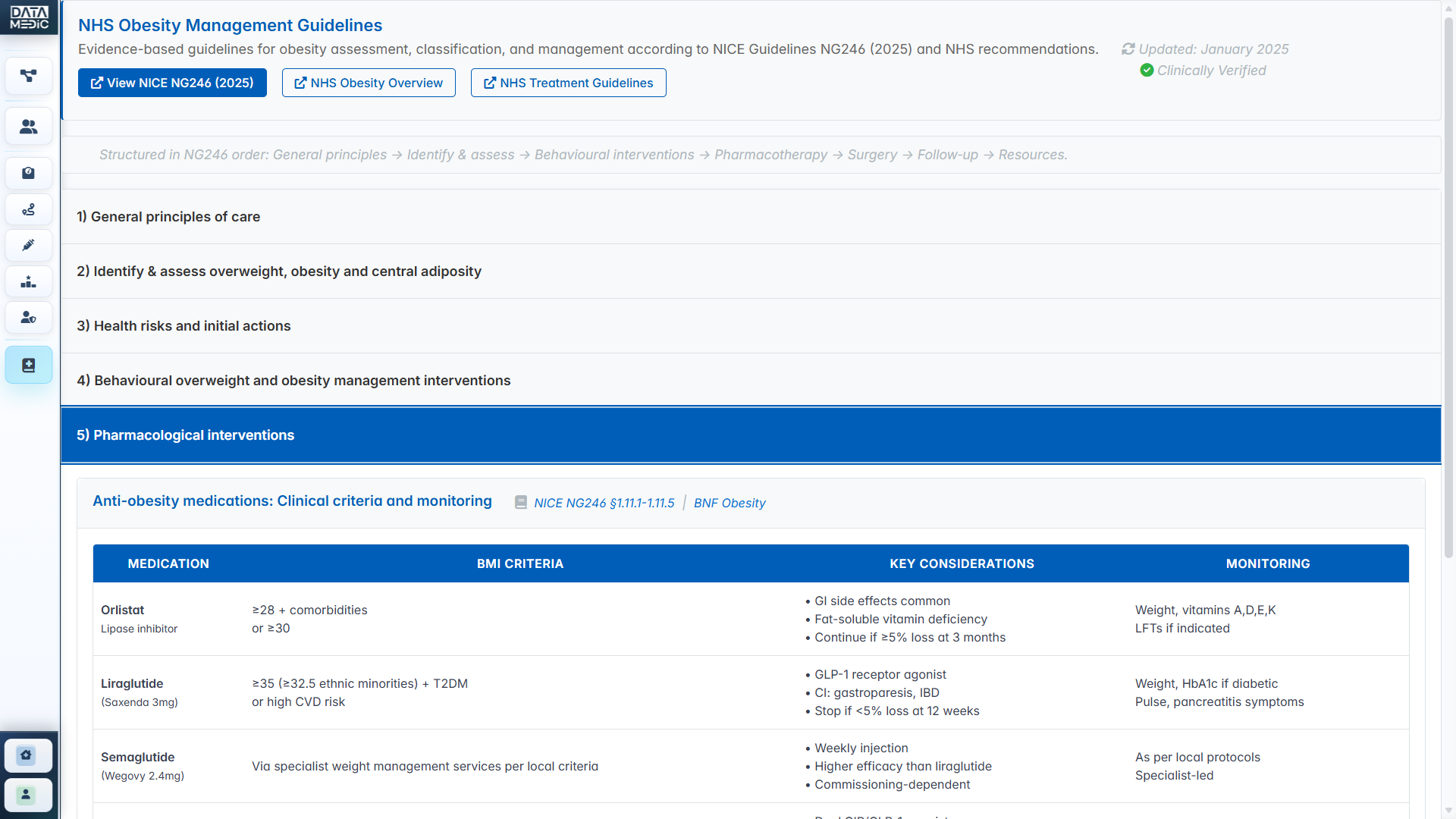
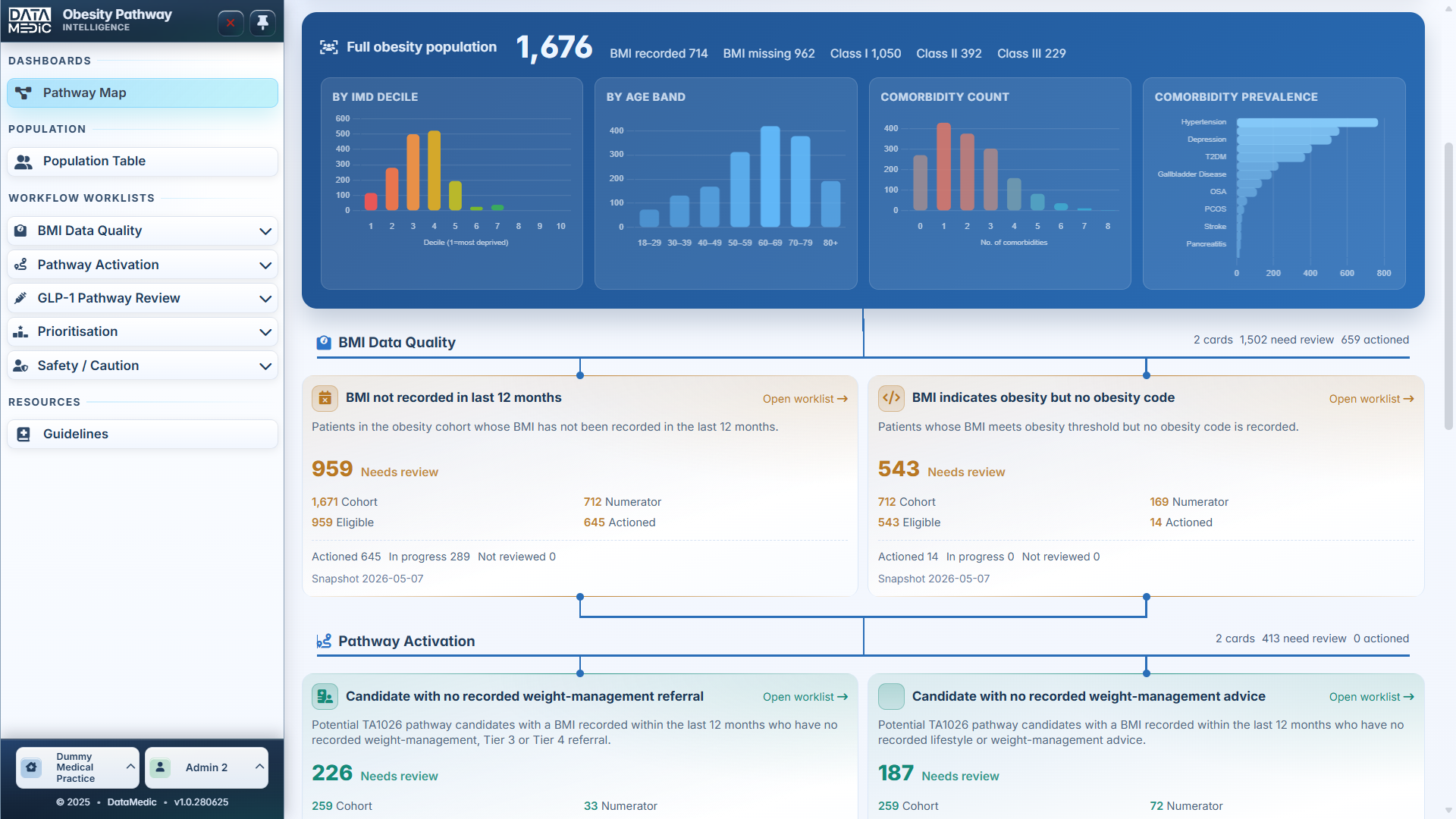
A workflow-led platform for NHS practices, PCNs and ICBs. Identify data quality gaps, activate weight-management pathways, review GLP-1/tirzepatide opportunity, prioritise high-need patients and surface safety/caution cohorts — all from one structured workspace.
312 patients in TA1026 review group
GLP-1 + DPP4 review · 18 patients